Fallen Arches Explained
Overview

A fallen arch or flatfoot is known medically as pes planus. The foot loses the gently curving arch on the inner side of the sole, just in front of the heel. If this arch is flattened only when standing and returns when the foot is lifted off the ground, the condition is called flexible pes planus or flexible flatfoot. If the arch disappears in both foot positions, standing and elevated, the condition is called rigid pes planus or rigid flatfoot.
Causes
Aging, injury, overuse, or illness can result in fallen arches or a fallen arch on one side. Diabetes. Obesity. Pregnancy. Nerve conditions. Foot abnormalities present since birth. Broken or dislocated bones in the foot. Stretched or torn tendons. Medical conditions such as arthritis. Sudden weight gain
Symptoms
Having flat feet can be painless and is actually normal in some people. But others with flat feet experience pain in the heel or arch area, difficulty standing on tiptoe, or have swelling along the inside of the ankle. They may also experience pain after standing for long periods of time or playing sports. Some back problems can also be attributed to flat feet.
Diagnosis
There are a few simple ways to assess your foot type, and most include making an imprint of your footprint. The classic way is to stand on a hard floor surface with wet feet to make a wet foot print. Look at the narrowest part of your footprint, which should be between your heel and ball of your foot. If the print of your foot in this part is less than 10% of the width of the widest part then you are likely to have high arches. more than 10% but less than 25% then your foot profile is probably normal, more than 25% or even the widest part, then you have flat feet.
pes planus exercises
Non Surgical Treatment
Custom orthotics are specially designed insoles, which are made for your by prescription. This is done by taking a plaster cast of the foot in its neutral position and is then sent to a laboratory, with your prescription to be made to your exact specifications. The insole then correctly aligns your foot and as a result your body. This will relieve abnormal strain of tissues and structures which can cause pain. For less severe mal-alignments or for sports use a wide variety of temporary insoles.
Surgical Treatment

This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Flat feet and fallen arches are common conditions that are in most cases asymptomatic. However, in patients who do have symptoms, treatments are available that can help reduce pain and promote efficient movement. Orthotic devices are well recognised as an excellent treatment and podiatrists can offer these different treatment modalities as individualised treatments for patients.
Prevention
Flatfeet in children are often an inherited family trait, but it may be possible to prevent the condition in some cases. Recent research has shown that there are several social or cultural factors that can cause flatfeet. These factors include the following, obesity, overweight, unnecessary orthopedic treatments, wearing rigid shoes at a young age, In 1992, a study in India of 2300 children aged 4-13 demonstrated a significant difference in the rate of flatfeet among those who wore shoes regularly and those who did not. In this study, wearing inflexible, closed-toe shoes in early childhood was shown to have a negative effect on the normal development of arches. Children who were allowed to go barefoot or who wore light sandals and slippers had a much lower rate of flatfeet. In 1999, a study in Spain of 1181 children aged 4-13 revealed that the use of orthopedic shoes for treatment of flatfeet in children not only failed to correct the problem, but actually worsened the condition by preventing the normal flexing and arch development of bare or lightly protected feet. Finally, in 2006, a study of 835 children aged 3-6 showed significant differences in the rate of flatfeet based on weight, with normal-weight children having lower rates of flatfeet than children who were overweight or obese. Among adults, flatfeet due to injury, disease, or normal aging are not preventable. However, when flatfeet are related to lifestyle factors, such as physical activities, shoe selection, and weight gain, careful attention to these factors may prevent the development of flatfeet.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.

A fallen arch or flatfoot is known medically as pes planus. The foot loses the gently curving arch on the inner side of the sole, just in front of the heel. If this arch is flattened only when standing and returns when the foot is lifted off the ground, the condition is called flexible pes planus or flexible flatfoot. If the arch disappears in both foot positions, standing and elevated, the condition is called rigid pes planus or rigid flatfoot.
Causes
Aging, injury, overuse, or illness can result in fallen arches or a fallen arch on one side. Diabetes. Obesity. Pregnancy. Nerve conditions. Foot abnormalities present since birth. Broken or dislocated bones in the foot. Stretched or torn tendons. Medical conditions such as arthritis. Sudden weight gain
Symptoms
Having flat feet can be painless and is actually normal in some people. But others with flat feet experience pain in the heel or arch area, difficulty standing on tiptoe, or have swelling along the inside of the ankle. They may also experience pain after standing for long periods of time or playing sports. Some back problems can also be attributed to flat feet.
Diagnosis
There are a few simple ways to assess your foot type, and most include making an imprint of your footprint. The classic way is to stand on a hard floor surface with wet feet to make a wet foot print. Look at the narrowest part of your footprint, which should be between your heel and ball of your foot. If the print of your foot in this part is less than 10% of the width of the widest part then you are likely to have high arches. more than 10% but less than 25% then your foot profile is probably normal, more than 25% or even the widest part, then you have flat feet.
pes planus exercises
Non Surgical Treatment
Custom orthotics are specially designed insoles, which are made for your by prescription. This is done by taking a plaster cast of the foot in its neutral position and is then sent to a laboratory, with your prescription to be made to your exact specifications. The insole then correctly aligns your foot and as a result your body. This will relieve abnormal strain of tissues and structures which can cause pain. For less severe mal-alignments or for sports use a wide variety of temporary insoles.
Surgical Treatment

This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Flat feet and fallen arches are common conditions that are in most cases asymptomatic. However, in patients who do have symptoms, treatments are available that can help reduce pain and promote efficient movement. Orthotic devices are well recognised as an excellent treatment and podiatrists can offer these different treatment modalities as individualised treatments for patients.
Prevention
Flatfeet in children are often an inherited family trait, but it may be possible to prevent the condition in some cases. Recent research has shown that there are several social or cultural factors that can cause flatfeet. These factors include the following, obesity, overweight, unnecessary orthopedic treatments, wearing rigid shoes at a young age, In 1992, a study in India of 2300 children aged 4-13 demonstrated a significant difference in the rate of flatfeet among those who wore shoes regularly and those who did not. In this study, wearing inflexible, closed-toe shoes in early childhood was shown to have a negative effect on the normal development of arches. Children who were allowed to go barefoot or who wore light sandals and slippers had a much lower rate of flatfeet. In 1999, a study in Spain of 1181 children aged 4-13 revealed that the use of orthopedic shoes for treatment of flatfeet in children not only failed to correct the problem, but actually worsened the condition by preventing the normal flexing and arch development of bare or lightly protected feet. Finally, in 2006, a study of 835 children aged 3-6 showed significant differences in the rate of flatfeet based on weight, with normal-weight children having lower rates of flatfeet than children who were overweight or obese. Among adults, flatfeet due to injury, disease, or normal aging are not preventable. However, when flatfeet are related to lifestyle factors, such as physical activities, shoe selection, and weight gain, careful attention to these factors may prevent the development of flatfeet.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.
Heel Aches
Overview

The heel bone is the largest of the 26 bones in the human foot. But while it is a large, strong bone, it is often injured, and this pain can be quite disabling at times. Heel pain can occur in the front, back, sides or bottom of the heel. That the heel is commonly injured is not surprising, perhaps, given the amazing amount of stress it must endure during a day. Indeed, it is one of the most common injuries of the foot; we see some variation of heel pain in our offices an average of 5 or 6 times per day.
Causes
While heel pain has many causes, it is usually the result of faulty biomechanics (abnormalities in the way we walk). This can place too much stress on the heel bone and the soft tissues attached to it. The stress may also result from injury, or a bruise incurred while walking, running or jumping on hard surfaces; wearing poorly constructed footwear; or being significantly overweight. Systemic diseases such as arthritis and diabetes can also contribute to heel pain. A common cause of heel pain is the heel spur, a bony growth under the heel bone. There are no visible features on the heel, but a deep painful spot can be found in or around the middle of the sole of the heel (see diagram). Approximately 10 per cent of the population may have heel spurs without any pain. Heel spurs result from strain on the muscles of the foot. This may result from biomechanical imbalance, a condition occurring in many people. Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation may be aggravated by shoes that lack appropriate support, especially in the arch area, and by the chronic irritation that sometimes accompanies an athletic lifestyle.Excessive rolling in of the feet when walking. An inflamed bursa (bursitis), a small, irritated sack of fluid at the back of the heel. A neuroma (a nerve growth). Other soft-tissue growths. Heel bumps or ?pump bumps?, a bone enlargement at the back of the heel bone. Bruises or stress fractures to the heel bone.
Symptoms
Usually worse with the first few steps in the morning or at the initial point of activity. The latter usually gets better with continued activity (squeaky hinge analogy). Walking, running, sprinting, hill running and jumping will increase the pain. Often, the natural response is to walk on the outside of the foot - in supination - to lessen the stress on the plantar fascia - resulting in new problems.
Diagnosis
Depending on the condition, the cause of heel pain is diagnosed using a number of tests, including medical history, physical examination, including examination of joints and muscles of the foot and leg, X-rays.
Non Surgical Treatment
Treatment of plantar fasciitis is usually performed in stages according to the duration and degree of pain. Treatment may take many months if the condition has been longstanding. Treatment usually begins with anti-inflammatory medication, shoe modification, temporary limitation of activities, weight loss and heel cord stretching. Also, night splints are often helpful to stretch the plantar fascia. An arch support (orthotic) may also be helpful, especially if you have a flat foot. If the problem continues, the tender area occasionally may be injected with cortisone and a local anesthetic. For a difficult, chronic problem, a period of casting may be used to improve this condition. Surgical treatment is rarely needed. If performed, it aims to partially release the plantar fascia and stimulate healing of the chronic inflammation. Removal of a heel spur, if it is large, may also be done at the time of surgery.
Surgical Treatment
With the advancements in technology and treatments, if you do need to have surgery for the heel, it is very minimal incision that?s done. And the nice thing is your recovery period is short and you should be able to bear weight right after the surgery. This means you can get back to your weekly routine in just a few weeks. Recovery is a lot different than it used to be and a lot of it is because of doing a minimal incision and decreasing trauma to soft tissues, as well as even the bone. So if you need surgery, then your recovery period is pretty quick.
replacement ankle straps for heels
Prevention

Wear shoes that fit well, front, back and sides and have shock-absorbent soles, rigid uppers and supportive heel counters. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm-up before running or walking, and do some stretching exercises afterward. Pace yourself when you participate in athletic activities. If overweight, try non weight-bearing activities such as swimming or cycling. Your podiatrist may also use taping or strapping to provide extra support for your foot. Orthoses (shoe inserts) specifically made to suit your needs may be also be prescribed.

The heel bone is the largest of the 26 bones in the human foot. But while it is a large, strong bone, it is often injured, and this pain can be quite disabling at times. Heel pain can occur in the front, back, sides or bottom of the heel. That the heel is commonly injured is not surprising, perhaps, given the amazing amount of stress it must endure during a day. Indeed, it is one of the most common injuries of the foot; we see some variation of heel pain in our offices an average of 5 or 6 times per day.
Causes
While heel pain has many causes, it is usually the result of faulty biomechanics (abnormalities in the way we walk). This can place too much stress on the heel bone and the soft tissues attached to it. The stress may also result from injury, or a bruise incurred while walking, running or jumping on hard surfaces; wearing poorly constructed footwear; or being significantly overweight. Systemic diseases such as arthritis and diabetes can also contribute to heel pain. A common cause of heel pain is the heel spur, a bony growth under the heel bone. There are no visible features on the heel, but a deep painful spot can be found in or around the middle of the sole of the heel (see diagram). Approximately 10 per cent of the population may have heel spurs without any pain. Heel spurs result from strain on the muscles of the foot. This may result from biomechanical imbalance, a condition occurring in many people. Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation may be aggravated by shoes that lack appropriate support, especially in the arch area, and by the chronic irritation that sometimes accompanies an athletic lifestyle.Excessive rolling in of the feet when walking. An inflamed bursa (bursitis), a small, irritated sack of fluid at the back of the heel. A neuroma (a nerve growth). Other soft-tissue growths. Heel bumps or ?pump bumps?, a bone enlargement at the back of the heel bone. Bruises or stress fractures to the heel bone.
Symptoms
Usually worse with the first few steps in the morning or at the initial point of activity. The latter usually gets better with continued activity (squeaky hinge analogy). Walking, running, sprinting, hill running and jumping will increase the pain. Often, the natural response is to walk on the outside of the foot - in supination - to lessen the stress on the plantar fascia - resulting in new problems.
Diagnosis
Depending on the condition, the cause of heel pain is diagnosed using a number of tests, including medical history, physical examination, including examination of joints and muscles of the foot and leg, X-rays.
Non Surgical Treatment
Treatment of plantar fasciitis is usually performed in stages according to the duration and degree of pain. Treatment may take many months if the condition has been longstanding. Treatment usually begins with anti-inflammatory medication, shoe modification, temporary limitation of activities, weight loss and heel cord stretching. Also, night splints are often helpful to stretch the plantar fascia. An arch support (orthotic) may also be helpful, especially if you have a flat foot. If the problem continues, the tender area occasionally may be injected with cortisone and a local anesthetic. For a difficult, chronic problem, a period of casting may be used to improve this condition. Surgical treatment is rarely needed. If performed, it aims to partially release the plantar fascia and stimulate healing of the chronic inflammation. Removal of a heel spur, if it is large, may also be done at the time of surgery.
Surgical Treatment
With the advancements in technology and treatments, if you do need to have surgery for the heel, it is very minimal incision that?s done. And the nice thing is your recovery period is short and you should be able to bear weight right after the surgery. This means you can get back to your weekly routine in just a few weeks. Recovery is a lot different than it used to be and a lot of it is because of doing a minimal incision and decreasing trauma to soft tissues, as well as even the bone. So if you need surgery, then your recovery period is pretty quick.
replacement ankle straps for heels
Prevention

Wear shoes that fit well, front, back and sides and have shock-absorbent soles, rigid uppers and supportive heel counters. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm-up before running or walking, and do some stretching exercises afterward. Pace yourself when you participate in athletic activities. If overweight, try non weight-bearing activities such as swimming or cycling. Your podiatrist may also use taping or strapping to provide extra support for your foot. Orthoses (shoe inserts) specifically made to suit your needs may be also be prescribed.
Functional Leg Length Discrepancy Symptoms
Overview
For discrepancies over five centimeters, more aggressive surgical procedures-specifically leg lengthening procedures-are typically required. The specifics of this operative procedure are beyond the scope of this informational page, but your child's physician will be able to discuss the details in reference to your child's specific problems when considered appropriate.
Causes
Some limb-length differences are caused by actual anatomic differences from one side to the other (referred to as structural causes). The femur is longer (or shorter) or the cartilage between the femur and tibia is thicker (or thinner) on one side. There could be actual deformities in one femur or hip joint contributing to leg length differences from side to side. Even a small structural difference can amount to significant changes in the anatomy of the limb. A past history of leg fracture, developmental hip dysplasia, slipped capital femoral epiphysis (SCFE), short neck of the femur, or coxa vara can also lead to placement of the femoral head in the hip socket that is offset. The end-result can be a limb-length difference and early degenerative arthritis of the hip.
Symptoms
Faulty feet and ankle structure profoundly affect leg length and pelvic positioning. The most common asymmetrical foot position is the pronated foot. Sensory receptors embedded on the bottom of the foot alert the brain to the slightest weight shift. Since the brain is always trying to maintain pelvic balance, when presented with a long left leg, it attempts to adapt to the altered weight shift by dropping the left medial arch (shortening the long leg) and supinating the right arch to lengthen the short leg.1 Left unchecked, excessive foot pronation will internally rotate the left lower extremity, causing excessive strain to the lateral meniscus and medial collateral knee ligaments. Conversely, excessive supination tends to externally rotate the leg and thigh, creating opposite knee, hip and pelvic distortions.
Diagnosis
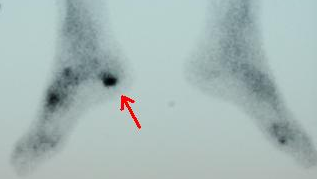
There are several orthopedic tests that are used, but they are rudimentary and have some degree of error. Even using a tape measure with specific anatomic landmarks has its errors. Most leg length differences can be seen with a well trained eye, but I always recommend what is called a scanagram, or a x-ray bone length study (see picture above). This test will give a precise measurement in millimeters of the length difference.
Non Surgical Treatment
Heel lifts and sole lifts are simple ways Pedorthists can compensate for leg length deficiencies. These small modifications can make a tremendous difference to a person?s comfort, balance and mobility. Although people do not always know if they have LLD if you have any of the symptoms I have mentioned you should consult a Pedorthist as treating your condition early will reduce the development of serious problems later on.

how do you get taller in a day?
Surgical Treatment
Surgical options in leg length discrepancy treatment include procedures to lengthen the shorter leg, or shorten the longer leg. Your child's physician will choose the safest and most effective method based on the aforementioned factors. No matter the surgical procedure performed, physical therapy will be required after surgery in order to stretch muscles and help support the flexibility of the surrounding joints. Surgical shortening is safer than surgical lengthening and has fewer complications. Surgical procedures to shorten one leg include removing part of a bone, called a bone resection. They can also include epiphysiodesis or epiphyseal stapling, where the growth plate in a bone is tethered or stapled. This slows the rate of growth in the surgical leg.
For discrepancies over five centimeters, more aggressive surgical procedures-specifically leg lengthening procedures-are typically required. The specifics of this operative procedure are beyond the scope of this informational page, but your child's physician will be able to discuss the details in reference to your child's specific problems when considered appropriate.

Causes
Some limb-length differences are caused by actual anatomic differences from one side to the other (referred to as structural causes). The femur is longer (or shorter) or the cartilage between the femur and tibia is thicker (or thinner) on one side. There could be actual deformities in one femur or hip joint contributing to leg length differences from side to side. Even a small structural difference can amount to significant changes in the anatomy of the limb. A past history of leg fracture, developmental hip dysplasia, slipped capital femoral epiphysis (SCFE), short neck of the femur, or coxa vara can also lead to placement of the femoral head in the hip socket that is offset. The end-result can be a limb-length difference and early degenerative arthritis of the hip.
Symptoms
Faulty feet and ankle structure profoundly affect leg length and pelvic positioning. The most common asymmetrical foot position is the pronated foot. Sensory receptors embedded on the bottom of the foot alert the brain to the slightest weight shift. Since the brain is always trying to maintain pelvic balance, when presented with a long left leg, it attempts to adapt to the altered weight shift by dropping the left medial arch (shortening the long leg) and supinating the right arch to lengthen the short leg.1 Left unchecked, excessive foot pronation will internally rotate the left lower extremity, causing excessive strain to the lateral meniscus and medial collateral knee ligaments. Conversely, excessive supination tends to externally rotate the leg and thigh, creating opposite knee, hip and pelvic distortions.
Diagnosis
There are several orthopedic tests that are used, but they are rudimentary and have some degree of error. Even using a tape measure with specific anatomic landmarks has its errors. Most leg length differences can be seen with a well trained eye, but I always recommend what is called a scanagram, or a x-ray bone length study (see picture above). This test will give a precise measurement in millimeters of the length difference.
Non Surgical Treatment
Heel lifts and sole lifts are simple ways Pedorthists can compensate for leg length deficiencies. These small modifications can make a tremendous difference to a person?s comfort, balance and mobility. Although people do not always know if they have LLD if you have any of the symptoms I have mentioned you should consult a Pedorthist as treating your condition early will reduce the development of serious problems later on.

how do you get taller in a day?
Surgical Treatment
Surgical options in leg length discrepancy treatment include procedures to lengthen the shorter leg, or shorten the longer leg. Your child's physician will choose the safest and most effective method based on the aforementioned factors. No matter the surgical procedure performed, physical therapy will be required after surgery in order to stretch muscles and help support the flexibility of the surrounding joints. Surgical shortening is safer than surgical lengthening and has fewer complications. Surgical procedures to shorten one leg include removing part of a bone, called a bone resection. They can also include epiphysiodesis or epiphyseal stapling, where the growth plate in a bone is tethered or stapled. This slows the rate of growth in the surgical leg.
Working with Mortons Neuroma
Overview
 Morton's neuroma (also known as Morton neuroma, Morton's metatarsalgia, Morton's neuralgia, plantar neuroma, intermetatarsal neuroma, and interdigital neuroma) is a benign neuroma of an intermetatarsal plantar nerve, most commonly of the second and third intermetatarsal spaces (between 2nd-3rd and 3rd-4th metatarsal heads), which results in the entrapment of the affected nerve. The main symptoms are pain and/or numbness, sometimes relieved by removing footwear.
Morton's neuroma (also known as Morton neuroma, Morton's metatarsalgia, Morton's neuralgia, plantar neuroma, intermetatarsal neuroma, and interdigital neuroma) is a benign neuroma of an intermetatarsal plantar nerve, most commonly of the second and third intermetatarsal spaces (between 2nd-3rd and 3rd-4th metatarsal heads), which results in the entrapment of the affected nerve. The main symptoms are pain and/or numbness, sometimes relieved by removing footwear.
Causes
Some say that this condition should not be called Morton's neuroma as, in fact, it is not actually a neuroma. A neuroma is a non-cancerous (benign) tumour that grows from the fibrous coverings of a nerve. There is no tumour formation in Morton's neuroma. The anatomy of the bones of the foot is also thought to contribute to the development of Morton's neuroma. For example, the space between the long bones (metatarsals) in the foot is narrower between the second and third, and between the third and fourth metatarsals. This means that the nerves that run between these metatarsals are more likely to be compressed and irritated. Wearing narrow shoes can make this compression worse.
Symptoms
Morton's neuroma may cause Burning, pain, tingling, and numbness often shooting into the toes. Discomfort that is worse while walking. Feeling of a lump between the toes. Symptoms are usually temporarily relieved when taking off shoes, flexing toes or rubbing feet.
Diagnosis
A GP (general practitioner, primary care physician) or a podiatrist (foot specialist doctor) will ask the patient to describe the pain as well as its intensity, when symptoms started, what types of shoes are worn, as well as some questions about their job, lifestyle and hobbies. The doctor will then examine the foot and try to locate the affected nerve. This may involve attempting to reproduce symptoms by manipulating the foot. In order to get a detailed image of the inside of the food, one of the following scans may be ordered. X-ray, this is a type of high-energy radiation. In low doses they are used to diagnose diseases and condition by making pictures of the inside of the body. In higher doses they are used to treat cancer. This procedure is non-invasive and painless. Ultrasound scan, high frequency sound waves are pointed at a specific part of the body, which in this case is the foot. The ultrasound waves bounce of tissues; their echoes are then converted into a picture, called a sonogram. This allows the doctor to get an inside view of the foot. This procedure is non-invasive and painless. MRI (magnetic resonance imagining) a device that uses a magnetic field and radio waves to create detailed images of the body. Unlike CT scanning or general x-ray studies, no ionizing radiation is involved with an MRI. This procedure is non-invasive and painless. The doctor will have to rule out other conditions which may have similar symptoms, including capsulitis, bursitis, or Freiberg's disease.
Non Surgical Treatment
If symptoms are severe or persistent and self-help measures did not help, the doctor may recommend corticosteroid injections, a steroid medication that reduces inflammation and pain is injected into the area of the neuroma. Only a limited number of injections are advised, otherwise the risk of undesirable side effects increases, including hypertension (high blood pressure) and weight gain. Alcohol sclerosing injections, studies have shown that alcohol injections reduce the size of Morton's neuromas as well as alleviating pain. This is a fairly new therapy and may not be available everywhere. The doctor injects alcohol in the area of the neuroma to help sclerose (harden) the nerve and relieve pain. Injections are typically administered every 7 to 10 days. For maximum relief 4 to 7 injections are usually needed.
Surgical Treatment
The above measures are often sufficient to resolve Morton?s Neuroma. Should the condition persist or worsen despite these efforts, surgery may be recommended to remove the Neuroma. The surgery requires only a short recovery period, though permanent numbness in the affected toes can result, so such surgery is generally used as a last resort.
 Morton's neuroma (also known as Morton neuroma, Morton's metatarsalgia, Morton's neuralgia, plantar neuroma, intermetatarsal neuroma, and interdigital neuroma) is a benign neuroma of an intermetatarsal plantar nerve, most commonly of the second and third intermetatarsal spaces (between 2nd-3rd and 3rd-4th metatarsal heads), which results in the entrapment of the affected nerve. The main symptoms are pain and/or numbness, sometimes relieved by removing footwear.
Morton's neuroma (also known as Morton neuroma, Morton's metatarsalgia, Morton's neuralgia, plantar neuroma, intermetatarsal neuroma, and interdigital neuroma) is a benign neuroma of an intermetatarsal plantar nerve, most commonly of the second and third intermetatarsal spaces (between 2nd-3rd and 3rd-4th metatarsal heads), which results in the entrapment of the affected nerve. The main symptoms are pain and/or numbness, sometimes relieved by removing footwear.Causes
Some say that this condition should not be called Morton's neuroma as, in fact, it is not actually a neuroma. A neuroma is a non-cancerous (benign) tumour that grows from the fibrous coverings of a nerve. There is no tumour formation in Morton's neuroma. The anatomy of the bones of the foot is also thought to contribute to the development of Morton's neuroma. For example, the space between the long bones (metatarsals) in the foot is narrower between the second and third, and between the third and fourth metatarsals. This means that the nerves that run between these metatarsals are more likely to be compressed and irritated. Wearing narrow shoes can make this compression worse.
Symptoms
Morton's neuroma may cause Burning, pain, tingling, and numbness often shooting into the toes. Discomfort that is worse while walking. Feeling of a lump between the toes. Symptoms are usually temporarily relieved when taking off shoes, flexing toes or rubbing feet.
Diagnosis
A GP (general practitioner, primary care physician) or a podiatrist (foot specialist doctor) will ask the patient to describe the pain as well as its intensity, when symptoms started, what types of shoes are worn, as well as some questions about their job, lifestyle and hobbies. The doctor will then examine the foot and try to locate the affected nerve. This may involve attempting to reproduce symptoms by manipulating the foot. In order to get a detailed image of the inside of the food, one of the following scans may be ordered. X-ray, this is a type of high-energy radiation. In low doses they are used to diagnose diseases and condition by making pictures of the inside of the body. In higher doses they are used to treat cancer. This procedure is non-invasive and painless. Ultrasound scan, high frequency sound waves are pointed at a specific part of the body, which in this case is the foot. The ultrasound waves bounce of tissues; their echoes are then converted into a picture, called a sonogram. This allows the doctor to get an inside view of the foot. This procedure is non-invasive and painless. MRI (magnetic resonance imagining) a device that uses a magnetic field and radio waves to create detailed images of the body. Unlike CT scanning or general x-ray studies, no ionizing radiation is involved with an MRI. This procedure is non-invasive and painless. The doctor will have to rule out other conditions which may have similar symptoms, including capsulitis, bursitis, or Freiberg's disease.
Non Surgical Treatment
If symptoms are severe or persistent and self-help measures did not help, the doctor may recommend corticosteroid injections, a steroid medication that reduces inflammation and pain is injected into the area of the neuroma. Only a limited number of injections are advised, otherwise the risk of undesirable side effects increases, including hypertension (high blood pressure) and weight gain. Alcohol sclerosing injections, studies have shown that alcohol injections reduce the size of Morton's neuromas as well as alleviating pain. This is a fairly new therapy and may not be available everywhere. The doctor injects alcohol in the area of the neuroma to help sclerose (harden) the nerve and relieve pain. Injections are typically administered every 7 to 10 days. For maximum relief 4 to 7 injections are usually needed.

Surgical Treatment
The above measures are often sufficient to resolve Morton?s Neuroma. Should the condition persist or worsen despite these efforts, surgery may be recommended to remove the Neuroma. The surgery requires only a short recovery period, though permanent numbness in the affected toes can result, so such surgery is generally used as a last resort.
How Shoe Lifts Remedy Leg Length Discrepancy
There are not one but two different types of leg length discrepancies, congenital and acquired. Congenital indicates that you are born with it. One leg is structurally shorter than the other. As a result of developmental periods of aging, the brain senses the gait pattern and identifies some variance. Your body usually adapts by tilting one shoulder to the "short" side. A difference of less than a quarter inch is not grossly irregular, demand Shoe Lifts to compensate and in most cases doesn't have a profound effect over a lifetime.

Leg length inequality goes mainly undiscovered on a daily basis, however this issue is easily solved, and can eliminate many incidents of chronic back pain.
Therapy for leg length inequality typically involves Shoe Lifts . These are very reasonably priced, ordinarily being less than twenty dollars, in comparison to a custom orthotic of $200 or even more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Upper back pain is easily the most common ailment afflicting people today. Over 80 million men and women are affected by back pain at some point in their life. It's a problem that costs companies millions of dollars yearly as a result of lost time and output. Fresh and better treatment solutions are continually sought after in the hope of decreasing the economical impact this condition causes.

People from all corners of the world experience foot ache due to leg length discrepancy. In these types of situations Shoe Lifts might be of very useful. The lifts are capable of alleviating any pain in the feet. Shoe Lifts are recommended by numerous skilled orthopaedic doctors.
To be able to support the human body in a healthy and balanced manner, your feet have a vital task to play. Despite that, it is sometimes the most neglected region in the body. Many people have flat-feet meaning there is unequal force exerted on the feet. This will cause other parts of the body such as knees, ankles and backs to be impacted too. Shoe Lifts guarantee that ideal posture and balance are restored.

Leg length inequality goes mainly undiscovered on a daily basis, however this issue is easily solved, and can eliminate many incidents of chronic back pain.
Therapy for leg length inequality typically involves Shoe Lifts . These are very reasonably priced, ordinarily being less than twenty dollars, in comparison to a custom orthotic of $200 or even more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Upper back pain is easily the most common ailment afflicting people today. Over 80 million men and women are affected by back pain at some point in their life. It's a problem that costs companies millions of dollars yearly as a result of lost time and output. Fresh and better treatment solutions are continually sought after in the hope of decreasing the economical impact this condition causes.

People from all corners of the world experience foot ache due to leg length discrepancy. In these types of situations Shoe Lifts might be of very useful. The lifts are capable of alleviating any pain in the feet. Shoe Lifts are recommended by numerous skilled orthopaedic doctors.
To be able to support the human body in a healthy and balanced manner, your feet have a vital task to play. Despite that, it is sometimes the most neglected region in the body. Many people have flat-feet meaning there is unequal force exerted on the feet. This will cause other parts of the body such as knees, ankles and backs to be impacted too. Shoe Lifts guarantee that ideal posture and balance are restored.
What Exactly Is Calcaneal Spur

Overview
Heel spur is a hook of bone that protrudes from the bottom of the foot where plantar fascia connects to the heel bone. Pain associated with heel spurs is usually pain from plantar fasciitis, not the actual bone. Heel spurs are most often diagnosed when a patient has visited a pain specialist or podiatrist for on-going foot pain related to plantar fasciitis; spurs are diagnosed via X-ray of the foot. Heel spurs are most commonly diagnosed in middle-aged men and women. As noted, most patients with this condition have other podiatry-related pain. This condition is a result of plantar fasciitis (when the fascia, a thick connective tissue that connects the heel bone and ball of the foot) becomes inflamed. Some 70% of plantar fasciitis patients have a bone spur. Bone spurs are soft calcium deposits caused from tension in the plantar fascia. When found on an X-ray, they are used as evidence that a patient is suffering from plantar fasciitis. Plantar fasciitis is typically caused from repetitive stress disorder. Walking, running, and dancing can cause this with time.
Causes
When a patient has plantar fasciitis, the plantar fascia becomes inflamed and degenerative (worn out)--these abnormalities can make normal activities quite painful. Symptoms typically worsen early in the morning after sleep. At that time, the plantar fascia is tight so even simple movements stretch the contracted plantar fascia. As you begin to loosen the plantar fascia, the pain usually subsides, but often returns with prolonged standing or walking.
Symptoms
Heel spur and plantar fasciitis pain usually begins in the bottom of the heel, and frequently radiates into the arch. At times, however, the pain may be felt only in the arch. The pain is most intense when first standing, after any period of rest. Most people with this problem experience their greatest pain in the morning, with the first few steps after sleeping. After several minutes of walking, the pain usually becomes less intense and may disappear completely, only to return later with prolonged walking or standing. If a nerve is irritated due to the swollen plantar fascia, this pain may radiate into the ankle. In the early stages of Heel Spurs and Plantar Fasciitis, the pain will usually subside quickly with getting off of the foot and resting. As the disease progresses, it may take longer periods of time for the pain to subside.
Diagnosis
A Diagnosis of Heel Spur Syndrome is a very common reason for having heel pain. Heel pain may be due to other types of conditions such as tendonitis, Haglund's Deformity, Stress Fracture, Tarsal Tunnel Syndrome, or low back problems. A more common condition in children is Sever's Disease. The diagnosis is usually made with a combination of x-ray examination and symptoms.
Non Surgical Treatment
The key for the proper treatment of heel spurs is determining what is causing the excessive stretching of the plantar fascia. When the cause is over-pronation (flat feet), an orthotic with rearfoot posting and longitudinal arch support is an effective device to reduce the over-pronation, and allow the condition to heal. Other common treatments include stretching exercises, losing weight, wearing shoes that have a cushioned heel that absorbs shock, and elevating the heel with the use of a heel cradle, heel cup, or orthotic. Heel cradles and heel cups provide extra comfort and cushion to the heel, and reduce the amount of shock and shear forces experienced from everyday activities.
Surgical Treatment
Surgery to correct for heel spur syndrome is a common procedure which releases plantar fascia partially from its attachment to the calcaneous (heel bone). This part of the surgery is called a plantar fasciotomy due to the fact the fascia is cut. This is most often done through an open procedure as any heel spur or bursa can be removed at the same time. If the spur is not removed during the surgery, it will probably be just as successful, as the large spur is not the true problem. Some physicians use an endoscopic approach (EPF) where a small camera aids the physician during surgery with typically smaller incisions on each side of your foot.
Prevention
Prevention of heel spur syndrome may be best by finding a good supportive shoe. Never go barefoot or wear a flat soled shoe. There are many over the counter arch supports that give increased support for your feet. Usually when there is excessive pronation the Achilles Tendon contracts or becomes shortened over time since it is not being used fully. The shortened Achilles Tendon is called an equinus deformity. By keeping this tendon stretched it may decrease some of the tension in the foot. Some theories believe the Achilles Tendon and plantar fascia is continuous. Before you get up from rest, stretch out your Achilles and the plantar fascia. You may attempt to spell the alphabet with your foot and ankle, use a towel against pressure on your foot, or roll a can of soup or sodapop on the ground. Ice may work well at the times of severe pain. For a chronic pain, or longer lasting pain heat therapy may improve the condition.
Just What Is Calcaneal Spur
Overview
The term heel spur generally refers more specifically to a heel spur, also known as a calcaneal spur. These calcium growths form around the tendons and ligaments of the foot and eventually become attached to the heel bone. The spurs then continue to grow, piercing the skin of the foot and causing pain and discomfort. When left untreated the spur can continue to grow causing agonizing pain and even immobilizing the patient.
Causes
Some causes of heel spurs include abnormal or lopsided walking, which places excessive stress on the heel bone, ligaments and nerves Running, jogging or jumping, especially on hard surfaces. Poorly fitted or badly worn shoes, especially those lacking appropriate arch support, excess weight and obesity.

Symptoms
You may or may not experience any symptoms with your heel spurs. It is normally the irritation and inflammation felt in the tissues around your heel spur that cause discomfort. Heel pain is one of the first things you may notice, especially when pushing off the ball of your foot (stretches the plantar fascia). The pain can get worse over time and tends to be stronger in the morning, subsiding throughout the day; although it does return with increased activity. A sharp, poking pain in your heel that feels like you're stepping on a stone can often be felt while standing or walking. You will sometimes be able to feel a bump on the bottom of your heel, and occasionally bruising may appear.
Diagnosis
A thorough history and physical exam is always necessary for the proper diagnosis of heel spurs and other foot conditions. X rays of the heel area are helpful, as excess bone production will be visible.
Non Surgical Treatment
Acupuncture and acupressure can used to address the pain of heel spurs, in addition to using friction massage to help break up scar tissue and delay the onset of bony formations. Physical therapy may help relieve pain and improve movement. The Feldenkrais method could be especially helpful for retraining some of the compensation movements caused by the pain from the spur. Guided imagery or a light massage on the foot may help to relieve some of the pain. Other treatments include low-gear cycling, and pool running. Some chiropractors approve of moderate use of aspirin or ibuprofen, or other appropriate anti-inflammatory drugs. Chiropractic manipulation is not recommended, although chiropractors may offer custom-fitted shoe orthotics and other allopathic-type treatments.
Surgical Treatment
In some cases, heel spurs are removed by surgery after an X-ray. While the surgery is typically effective, it?s a timely and expensive procedure. Even after surgery, heel spurs can re-form if the patient continues the lifestyle that led to the problem. These reasons are why most people who develop painful heel spurs begin looking for natural remedies for joint and bone pain. Surgery isn?t required to cure a heel spur. In fact, more than 90 percent of people get better with nonsurgical treatments. If nonsurgical methods fail to treat symptoms of heel spurs after 12 months, surgery may be necessary to alleviate pain and restore mobility.